Supporting Brain Health During Menopause: Understanding the Role of Technology
This report explores how menopause affects women’s brain health and highlights the growing role of technology in supporting cognitive and mental well‑being. Created in partnership with leading women's health-focused researchers and organizations, it offers market intelligence for innovators, researchers, healthcare leaders, investors, and policymakers working at the intersection of aging, women’s health, and technology.

CABHI’s AgeTech Insights provides market intelligence into the evolving needs and priorities of populations across the lifespan, with a focus on aging, brain health, and technology. By centering lived experience and encouraging co-design approaches, AgeTech Insights aims to connect innovators, researchers, policymakers, and communities to support the development of inclusive and impactful agetech policies, products, and practices.
Menopause represents a critical yet under-addressed period for women’s cognitive and mental health, occurring at a life stage when many women remain active in the workforce, caregiving, and community life. While primarily considered a later-life event, menopause can occur at any reproductive age due to surgical removal of the ovaries, premature ovarian insufficiency, and chemotherapy (to name a few). Awareness of menopause-related cognitive and mental health changes is increasing, yet women continue to report limited access to timely, trustworthy, and integrated support. These gaps have implications not only for individual wellbeing, but also for population health, healthcare system demand, and economic impact, particularly as Canada’s population ages. This report was developed in response to a clear mismatch between women’s interest for technology-enabled support and the limited availability of menopause-informed, evidence-based digital solutions that are integrated into care pathways and lifestyle interventions.
This report is the result of a collaborative effort between CABHI and FemTech Canada; the Einstein Lab of Cognitive Neuroscience, Gender, and Health at the University of Toronto; the Galea Laboratory of Behavioural Neuroendocrinology at the Centre for Addiction and Mental Health; the Rajah Laboratory for Brain Health Equity in Aging and Memory at Toronto Metropolitan University; Women’s Age Lab at Women’s College Hospital; and the Women’s Brain Health Initiative.
Each partner contributed complementary expertise to strengthen the scientific rigor, equity focus, and real-world relevance of the report. Academic research partners--including the Galea Laboratory, Einstein Lab, Rajah Laboratory, and Women’s Age Lab--ensure that the findings are grounded in current evidence from neuroscience, neuroendocrinology, cognitive aging, and women’s health research. Their involvement supports alignment with best practices in evidence-informed care and interpretation.
Women’s Brain Health Initiative brings a public health and knowledge translation perspective, supporting the development of accessible and evidence-based information for women across the lifespan. FemTech Canada contributes policy and advocacy expertise, helping ensure that the findings of this report reach all women with menopause including older persons, innovators, and decision-makers working to advance women-centred health technologies.
The integration of research, policy, and innovation perspectives underscores a shared commitment to improving women’s brain health across early- and later-midlife and older adulthood, and reflects the importance of bridging evidence, lived experience, and technology development.
CABHI is proud to work alongside its partners to advance understanding in this area and to support innovators, healthcare systems, and policymakers in responding to identified gaps. Findings such as those presented in this report contribute to informed decision-making, inclusive innovation, and sustained investment in solutions that support women’s health and wellbeing across the lifespan.
Dr. Negar Mazloum-Farzaghi, Lead Writer and Co-Principal Investigator for the AgeTech Insights Reports and Knowledge Broker at the Centre for Aging + Brain Health Innovation
Dr. Allison Sekuler, Co-Principal Investigator for the AgeTech Insights Reports and President and Chief Scientist at the Centre for Aging + Brain Health Innovation
James Mayer, Co-Principal Investigator for the AgeTech Insights Reports and Chief Operating Officer at the Centre for Aging + Brain Health Innovation.
High awareness of menopause-related brain health changes
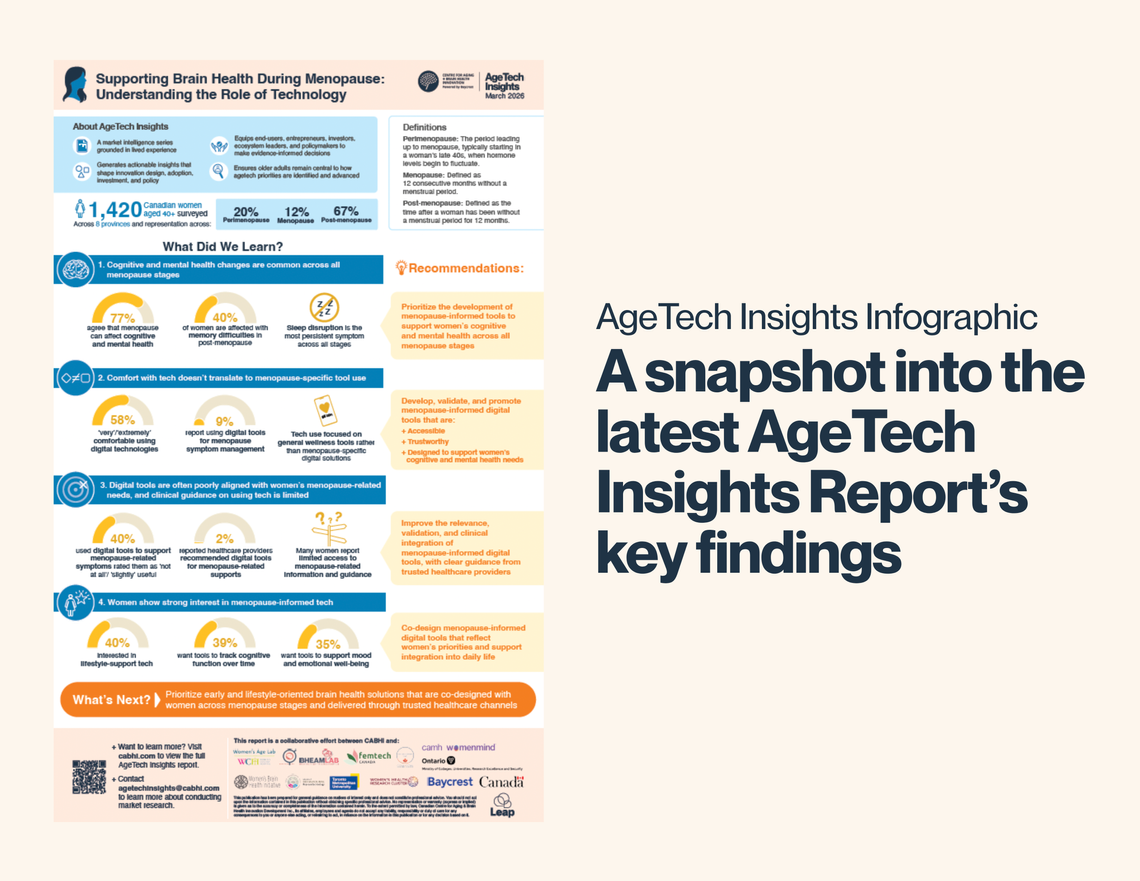
Overall awareness of menopause-related cognitive and mental health changes was high. Seventy-seven percent of respondents agreed that symptoms such as memory difficulties, trouble concentrating, mood changes, and sleep disturbances can occur during any type or stage of menopause.
Sleep and cognitive symptoms persist across menopause types and stages
Cognitive and mental health symptoms were common across all menopause types and stages, with sleep disturbances emerging as the most prevalent concern. During perimenopause, 57% of respondents reported sleep problems. This peaked at 58% during menopause and remained high in post-menopause (54%). Memory difficulties were reported by 32% during perimenopause, 29% during menopause, and 40% during post-menopause. Trouble concentrating (“brain fog”) affected 36%, 33%, and 27% of respondents across perimenopause, menopause, and post-menopause, respectively.
High digital comfort but limited technology use
The use of digital technologies to manage menopause-related cognitive or mental health symptoms remains limited. Nearly half of women (49%) reported not using any digital tools for symptom management, even though 58% reported being very or extremely comfortable using digital technologies. Among those who reported technology use, engagement focused on general wellness tools rather than menopause-specific digital solutions. The most commonly used tools included fitness or wellness apps and wearables (28%), sleep trackers (18%), and meditation or mindfulness apps (16%), while use of menopause symptom trackers remained low (4%).
Mixed perceptions of technology effectiveness
Perceptions of technology effectiveness were mixed. Among users, 40% rated digital tools as ‘not at all’ or only ‘slightly’ useful for managing symptoms, and 21% rated them as ‘very’ or ‘extremely’ useful. Using technology to access educational resources about menopause-related cognitive and mental health changes was similarly modest. Twenty-one percent of respondents reported using health websites, even fewer reported engagement with podcasts, webinars, apps, or online programs (5%), and 26% reported not using any technology for this purpose.
Minimal clinical integration and ongoing care delivery gaps highlight one of the biggest opportunities for technologies in this space
Integration of digital tools into healthcare practices remains minimal. Only 2% of respondents reported that a healthcare provider had recommended technology to support cognitive or mental health during any type or stage of menopause. Many respondents also identified gaps in care, including lack of information or education about cognitive changes (30%), limited access to providers with specialized menopause training (24%), insufficient guidance from healthcare professionals (27%), dismissal or minimization of symptoms (19%), and difficulty finding trustworthy information (18%).
Clear opportunity for menopause-focused tech solutions
Overall, these findings show that while women experience a high symptom burden and are comfortable using digital technologies, they are largely relying on tools not designed for menopause (e.g., general wellness apps or sleep trackers). As a result, these technologies often fail to provide adequate support for managing menopause-related health concerns. This gap highlights the need for menopause-informed, clinically integrated tech solutions that are designed around women’s biology and lived experience, rather than requiring women to adapt to systems and technologies not built for them.
Key Findings
Below is a high-level summary of key findings + learnings. To dive deeper, download the full report.
-
Menopause-related cognitive and mental health changes are widely reported and experienced
Sleep disturbances, brain fog, memory issues, and mood symptoms affect women across all stages. Awareness is already high—what’s missing is action.
-
Sleep and cognitive symptoms persist across the menopause types and stages
Sleep and cognitive symptoms do not peak in one stage; they continue across perimenopause through post‑menopause, indicating the need for long‑term support.
-
Concern about cognitive decline is common across menopause types and stages
Over one‑third of women worry about dementia or long‑term memory loss, driven by lived experience of cognitive changes.
-
Non-medical coping strategies dominate, and menopause hormone therapy use is limited
Exercise and talking to peers are the most common coping tools. Medical treatments like hormone therapy are far less used.
-
Technology remains underused for symptom management and education
Nearly half of women experiencing symptoms do not use any digital tools, and most who do rely on general wellness apps—not menopause‑specific ones.
-
Perceived value of existing technologies is modest
Many women find digital tools minimally useful, suggesting a mismatch between available features and their real needs.
-
Technology interest is high
Despite low current uptake, most women say they would use menopause‑informed tools, especially those focused on sleep, mood, cognition, and lifestyle support.
-
Healthcare guidance on digital tools is largely absent
Only 2% of women report receiving tech recommendations from healthcare providers, reflecting a major gap in clinical integration.


Overall Recommendation

Discussion

I feel I can manage the changes happening within my body as I age, but the real challenge is the social context that creates barriers to symptom management and healthy living for women. Unrealistic work demands, managing family responsibilities (caregiving for older adults and young children at the same time), and being told to prioritize ‘self-care’ make this especially difficult, while struggles are often framed as personal failings rather than a lack of adequate supports. Flexible working environments and reasonable workloads would go a long way toward making life more bearable at this stage of my life.
Survey respondent

Recommendations
-
Develop tools to track and manage cognitive, mental, and physiological symptoms
Design menopause-informed cognitive tools that combine symptom tracking with clear, actionable pathways to care, including education about treatment options and streamlined access to qualified healthcare providers. Menopause-specific digital solutions should function as gateways to care, helping women identify when symptoms warrant clinical assessment, enabling timely referral to menopause-trained providers, and supporting informed discussions about treatment options, including medications where appropriate.

-
Integrate lifestyle support into menopause-focused technologies
Build integrated platforms that connect lifestyle tracking with cognitive and mental health insights, rather than offering isolated features.
-
Address sleep as a core component of cognitive and mental health support
Develop menopause-informed sleep solutions that combine tracking, education, and actionable guidance linked to cognitive and emotional well-being.
-
Expand education on menopause and brain health
Develop educational tools tailored to different users—including women, clinicians, and employers—with content adapted to life stage, symptoms, and user goals. Tools should incorporate credible menopause and brain health expertise and be designed for integration into existing health, training, and workplace systems, including recommendation by primary care providers and OB-GYNs.
-
Strengthen access through telehealth and healthcare-backed tools
Support the integration and scale of evidence-informed, clinically grounded technologies by strengthening pathways for provider recommendation and system-level adoption. Solutions should be embedded within telehealth and routine care workflows, supported by clear clinical guidance, and positioned for coverage within standard insurance and employer health benefit packages.